Macular Degeneration
What is macular degeneration?
It is a condition which can affect the central vision and is more common over the age of 50. There are 2 forms: dry and wet macular degeneration.
Who is at risk for macular degeneration?
The main risk factors are age and family history (genetics). Other risk factors are discussed below.
What treatment is there for macular degeneration?
Different treatments exist depending on the type of macular degeneration. See below for more details.
What is macular degeneration?
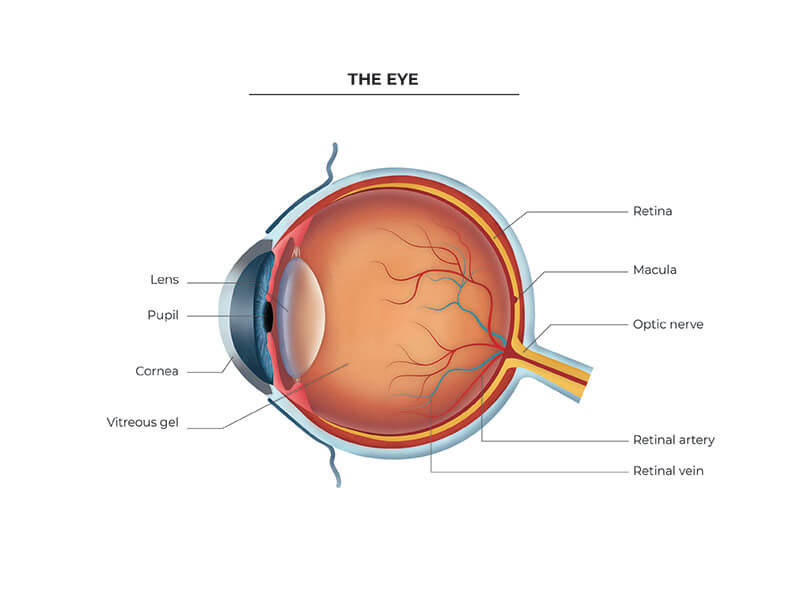
Age-related macular degeneration (AMD) is a disease that affects the central vision you need for “straight-ahead” activities such as reading and driving. The macula is the name given to the centre of the retina, and is the area where all fine detailed vision is processed. AMD affects the macula, the part of the eye that allows you to see fine detail. It does not cause any pain and it does not affect your peripheral vision. In some cases, AMD advances so slowly that people notice little change in their vision. In others, it may progress faster and lead to a decrease in central vision. It is currently a leading cause of vision loss in patients 60 years and older.
What are dry and wet macular degeneration?
Dry AMD occurs when the light-sensitive cells in the macula slowly degenerate, gradually blurring central vision in the affected eye. As dry AMD progresses, you may notice a blurred spot in the centre of your vision. Over time, central vision in the affected eye may become more affected. This form of AMD generally affects both eyes, but one eye can be more affected than the other.
Wet AMD occurs when abnormal blood vessels grow from the choroid (the layer between the retina and sclera) into the retina. These new blood vessels are fragile and often leak blood and fluid. The fluid raises the macula from its normal position and causes damage to the photoreceptors, which do not function well in a fluid-filled environment. Visual decline is noted rapidly, often over weeks. Wet AMD is considered to be advanced AMD and is more severe than the dry form.
Dry AMD is much more common than wet AMD. More than 85% of all people with AMD will have the dry form only. However in those with significant vision loss from AMD approximately two thirds of patients will have the wet form. All people who have the wet form will have the dry form first. The dry form can also advance and cause vision loss without turning into the wet form even during the early stages of AMD. There is currently no way to predict if or when a dry form will turn into the wet form.
Who is at risk for macular degeneration?
The main risk factors for AMD are age and family history (genetics). Women appear to be at greater risk than men. The only modifiable risk factors are smoking, obesity and high blood pressure so these should be addressed to decrease your risk of vision loss.
An amsler grid should be used to watch for a change in vision and may suggest that wet AMD is developing. The pattern of the grid resembles a chequerboard. You will cover one eye and stare at the black dot in the centre of the grid at a distance of 30cm. While staring at the dot, you may notice that straight lines in the pattern appear wavy. Sudden changes in the grid appearance should be reported to your eye specialist.
Dry macular degeneration treatment
The National Eye Institute’s age-related eye disease study (AREDS) found that taking a specific high dose formulation of antioxidants and zinc significantly reduces the risk advanced AMD and its associated vision loss. Slowing AMD’s progression from the intermediate stage to the advanced stage is currently the mainstay of treatment for patients with dry AMD. The specific daily amounts are based on the AREDS and AREDS 2 research.
This formulation is not a cure for AMD. It will not restore vision already lost from the disease. However, it may delay the onset of advanced AMD. The high levels of vitamin C and minerals are difficult to achieve from diet alone. However, previous studies have suggested that people who have diets rich in green leafy vegetables have a lower risk of developing AMD. In addition, the levels of antioxidants and zinc are considerably higher than the amount in any daily multi-vitamin. A multivitamin contains many important vitamins not found in the AREDS formulation. You may want to take a multivitamin along with the AREDS formulation. If you are taking more than 1 multivitamin, speak to your general practitioner about the cumulative dosage of the vitamins.
Wet macular degeneration treatment
The mainstay of treatment for wet AMD is intravitreal injections. These are special medicines which cause the abnormal blood vessels under the retina to shrink, but not permanently disappear. This allows the fluid under the retina to subside and the vision to improve. These injections have been shown to be very effective in preventing further vision loss and often allow improvement of vision. Unfortunately, these injections are treatments rather than a cure for AMD and you will require multiple injections on an ongoing basis. In some cases, the disease and loss of vision may progress despite treatment. The type of treatment and possibility for treatment depends on characteristics of the wet AMD and will be discussed with you by your doctor.
Your lifestyle can play a role in reducing your risk of developing AMD. Eat a healthy diet high in green leafy vegetables and fish. Don’t smoke, maintain normal blood pressure and maintain a healthy body weight with regular exercise.
What happens during the eye injections?
Anaesthetic drops will be placed to anaesthetise the surface of your eye. A speculum is used to hold your eye open. An iodine solution is placed on the surface of your eye to sterilise it. You will be asked to look at or behind you to correctly rotate your eyes. The medicine will then be injected. It is normal to feel a pinch or pressure at the time of the injection. Any discomfort is usually temporary. The remaining iodine solution will then be flushed from your eyes. It is normal for the eye to be slightly red after the procedure. Each injection carries a small risk for infection which can be detrimental to vision. New temporary eye floaters are also common. If you have any questions, do not hesitate to ask.
Frequently Asked Questions
What is the best eye vitamin for macular degeneration?
Antioxidants and zinc have been found to assist in decreasing the risk of macular degeneration. To reach the mineral levels needed to delay the onset or progression of macular degeneration, specifically formulated supplements, in addition to daily multi-vitamins, are usually required. Ask your ophthalmologist about vitamin supplementation and diet in macular degeneration.
What is the best treatment for macular degeneration?
Specifically formulated doses of antioxidants and zinc can assist in decreasing the risk and progression of dry AMD. Additionally diets rich in green, leafy vegetables can help to lower the risk of developing AMD. The primary treatment for wet AMD is intravitreal injections.
How long does macular degeneration take to progress?
The progression of AMD varies from person to person. For some it progresses very slowly and, as there is no pain associated with it, can go unnoticed for a long time. For others it progresses rapidly and their loss of central vision is quickly noticeable.
Can you prevent macular degeneration?
Decreasing the risk of developing as well as the progression of AMD is possible by maintaining a healthy lifestyle. Specifically, by not smoking, keeping a healthy weight and blood pressure, eating leafy green vegetables and taking specifically formulated supplements high in antioxidants and zinc.