Retinal Detachment Surgery
What is a retinal detachment?
The retina is a thin layer of tissue at the back of the eyeball which contains the rods and cones. These light-sensitive cells absorb light and trigger nerve impulses which pass via the optic nerve to the brain, where the visual image is formed.
What are symptoms of a retinal detachment?
The initial symptoms of a retinal detachment may be quite mild. A sudden onset of flashing lights and multiple new floaters (like “cobwebs” or specs that float about in your field of vision) may occur. Flashes and floaters are often the symptoms of a retinal tear.
How is a retinal detachment repaired?
A retinal detachment can only be repaired with a surgical procedure. There are three main types of surgical procedures for retinal detachment repair…
What is a retinal detachment?
The retina is a thin layer of tissue at the back of the eyeball which contains the rods and cones. These light-sensitive cells absorb light and trigger nerve impulses which pass via the optic nerve to the brain, where the visual image is formed. A retinal detachment is the loosening or separation of this layer from the underlying structures in the eye and is primarily due to traction or pulling of the vitreous gel on the retina.
As we age, a physiological process called a ‘posterior vitreous separation’ takes place, in which the vitreous gel separates itself from the retina. During this separation, the gel may pull on the retina, causing a retinal tear and allowing fluid to access the space behind the retina and detach it. A retinal detachment is an urgent condition which can result in permanent visual loss if untreated. Fortunately, most retinal detachments are treatable with surgery.
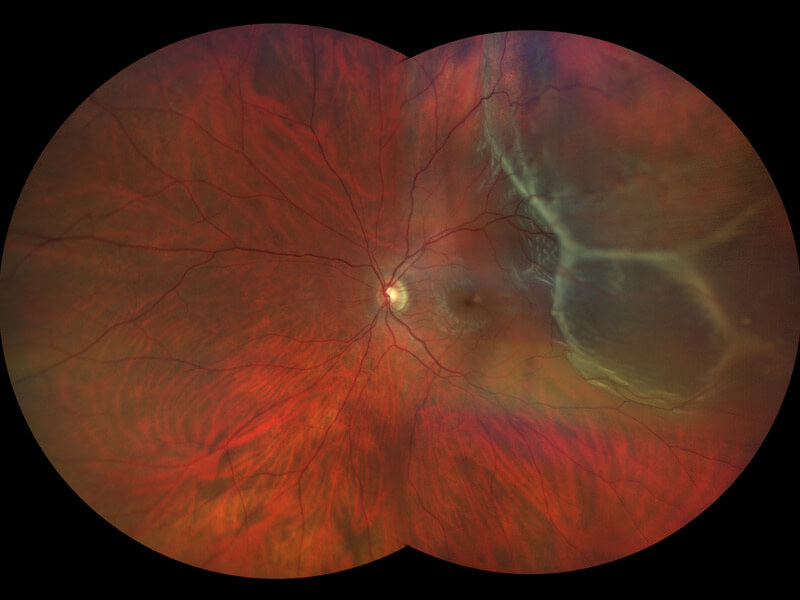
Photograph of a left retina showing a retinal detachment. This condition is an emergency which requires surgery.
What are symptoms of a retinal detachment?
The initial symptoms of a retinal detachment may be quite mild. A sudden onset of flashing lights and multiple new floaters (like “cobwebs” or specs that float about in your field of vision) may occur. Flashes and eye floaters are often the symptoms of a retinal tear.
After a retinal tear has occurred the retina may begin to detach. As the retina starts to detach, changes in the peripheral vision (outside vision) in the affected eye begin to occur.
Loss of peripheral vision from the top or bottom may advance towards the centre of the vision like a black curtain, often in a half-moon shape. This can progress to total vision loss. Sometimes, the symptoms of a retinal detachment may go unnoticed until the central vision is affected.
Who is at risk?
A retinal detachment can occur at any age,but it is more common in people over the age of 40.
Risk factors for retinal detachment include:
- Myopia (nearsightedness)
- Previous retinal detachment in the fellow eye
- Family history of retinal detachment
- Cataract operation
- Eye trauma
- Predisposing genetic conditions
- Other predisposing eye diseases or disorders
How is a retinal detachment repaired?
A retinal detachment can only be repaired with a surgical procedure. There are three main types of surgical procedures for retinal detachment repair:
1. Pars plana vitrectomy
This is the most common form of retinal detachment surgery. Three small incisions are made through the sclera (the white of the eye). A microscope and a special viewing system are used to operate directly in the eye. A special instrument, called a vitrector, is used to remove the vitreous gel. This eliminates the traction on the retina.
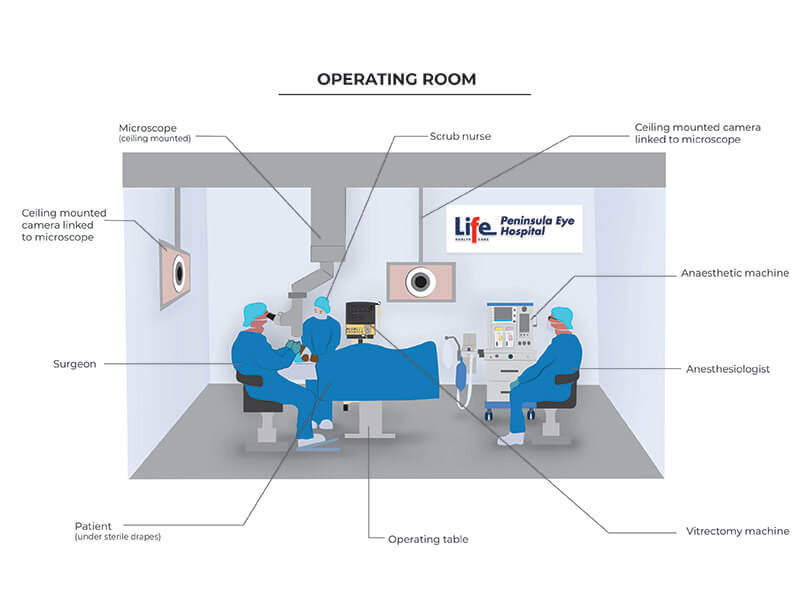
Image of surgery being performed at Peninsula Eye Hospital for a retinal detachment repair.
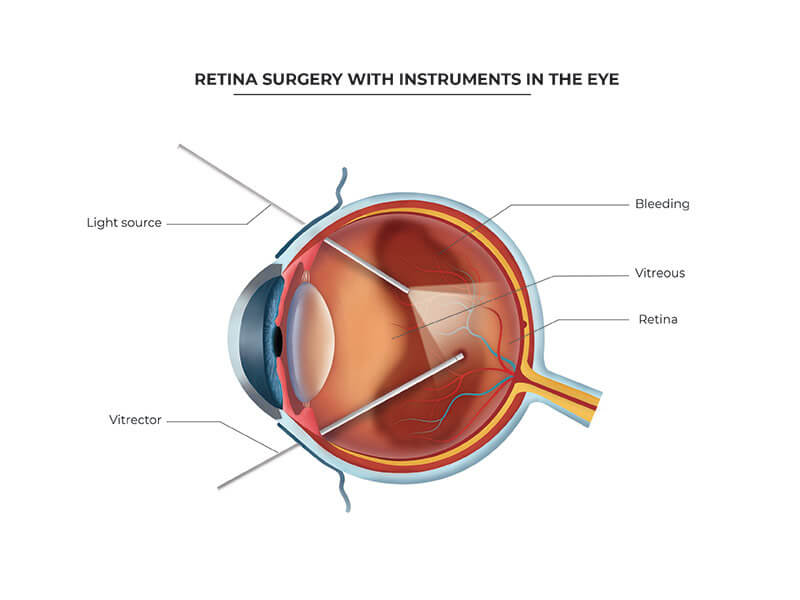 Image of vitrectomy instruments and light source during vitrectomy surgery.
Image of vitrectomy instruments and light source during vitrectomy surgery.
The fluid under the retina is drained and laser is applied around the retinal break to permanently seal it off. A tamponade agent (gas or silicone oil) is then injected into the eye to fill the vitreous cavity.
When a gas bubble is placed, the surface tension of the gas acts to seal off the retinal breaks while the laser spots are maturing. You may be asked to position your head in a specific way after surgery to ensure the gas bubble is covering the retinal breaks. The gas bubble will slowly be absorbed by your eye at different rates depending on the type of gas used.
Sometimes silicone oil is placed within the vitreous cavity instead of gas. In this case, a second surgery is usually required to remove the oil. Sometimes a combination of both a scleral buckle and vitrectomy surgery may be required.
2. Scleral buckle
In this procedure, a silicone band is placed around the outside of the eye behind the insertion of the four major muscles that move the eye. This imbricates the eye wall to move it closer to the retina. This acts to release the pulling of the vitreous gel on the retina to allow closure of the retinal breaks. Cryotherapy is placed around the retinal breaks during the procedure to create a permanent adhesion between the retinal break and underlying tissue.
Fluid may then be removed through a small incision in the sclera to decrease to flatten the retina. Finally, a temporary gas bubble is injected into the eye. The surface tension of the gas bubble acts to seal off the retinal tear.
3. Pneumatic retinopexy
This procedure is only used to treat retinal detachments with very specific characteristics. A temporary gas bubble is injected into the vitreous cavity of the eye. The surface tension of the gas bubble acts to seal off the retinal tear. Laser or cryotherapy may be placed during or after the procedure.
The success of this procedure requires strict positioning of your head after the gas injection to ensure the bubble seals of the retinal break.
Which intraocular tamponades may be used?
Gas
Gas placed within the eye will be gradually reabsorbed by the eye over a 2 to 8 week period following surgery, depending on the type of gas used. As the bubble is reabsorbed, the vitreous cavity refills with the fluid that is naturally produced by the eye. Vision will be markedly reduced immediately after surgery since you cannot see well through a bubble.
As the bubble is reabsorbed you will gradually see more and more. You may not fly in an aeroplane or travel to any elevation above sea level until the bubble is completely gone. Some types of general anaesthetic agents must be avoided (nitrous oxide) while there is a gas bubble in the eye.
Silicone Oil
Silicone oil does not reabsorb on its own; instead it must be removed with an additional surgical procedure. It is reserved for cases where the retinal detachment requires a longer time to heal, or where gas is deemed insufficient due to travel or work circumstances.
Is laser used to treat a retinal detachment?
Yes, laser treatment is used during the retinal detachment surgery to create an adhesion between the retina and underlying tissues around the retinal tear or retinal break. The retinal laser is used in conjunction with surgery and is not performed in isolation during a retinal detachment repair. In some cases (like in scleral buckle surgery) cryotherapy is used instead of laser. The laser takes time to create an adhesion with the underlying tissue, and this is the reason a tamponade agent (gas bubble or silicone oil) is placed in the eye, allowing the retinal laser to take full effect so the retina may heal.
How long does recovery take post retinal detachment surgery?
This depends on several factors, including the configuration of the retinal detachment and the amount of scar tissue the eye has produced. You can expect to be off work for 2 weeks. You may be expected to position your head for 5 to 7 days to allow the gas bubble or silicone oil to press against a certain part of the retina while it heals. Some eye floaters can be expected after the retinal detachment surgery, but these are usually transient and subside over a few weeks.
The single operation success for retinal detachment repair in an acute (no signs of chronicity) retinal detachment is approximately 85%. The reason for this is due to the scar tissue the eye produces when it heals following a retinal detachment. The visual recovery time (sight) following a retinal detachment repair is not always predictable and the final visual result will only be known several months following surgery.
It is recommended to refrain from all exercise for 2 weeks following a retinal detachment repair. During this time, head positioning and rest are very important for a favourable outcome. Between week 2 and week 4 following retinal detachment surgery, you can gradually start resuming normal activities, and 1 month after surgery all activity restrictions are usually lifted.
You will be given eye drops to take home. These include steroid eye drops to control inflammation and antibiotic eye drops to prevent infection.
Driving after a retinal detachment repair and its requirements will differ depending on the type and configuration of the detachment, and whether gas or silicone oil is used to treat the detachment. This will be discussed with you in detail before the operation.
Frequently Asked Questions
How do you check for retinal detachment?
Ophthalmologists check for retinal detachment by examining the eye with specialised equipment that uses a combination of light and lenses, thereby enabling them to visualise the entire retina. If there is bleeding in the eye, they may use ultrasound imaging to assess the integrity of the retina.
Can dry eyes cause retinal detachment?
Dry eyes cannot cause a retinal detachment. This is because a retinal detachment occurs at the back of the inside of the eye. It is caused by the loosening or separation of the retina from the underlying structures when the vitreous gel pulls on the retina.
How is a retinal detachment treated?
Retinal detachments do not heal by themselves. This condition is serious and without treatment can result in permanent loss of vision. However, as most retinal detachments can be repaired through surgery it can usually be successfully repaired by an ophthalmologist.
What is the most common cause of retinal detachment?
Retinal detachment is most often caused by a posterior vitreous detachment, which is an age related process. It is more common in people over 40 years of age, although it can occur at any age. Additional risk factors include myopia (near-sightedness), a previous retinal detachment in the other eye and a family history of retinal detachment.
How long does it take for vision to improve after retinal detachment surgery?
The timing for visual improvement is quite variable and depends on several factors, including the type of retinal detachment, duration and whether the macula has been involved. It is also dependent on how much scar tissue the eye produces and how long the detachment has been present.
Download Dr Lapere’s abstract study Vitrectomy and injection of subretinal tissue plasminogen activator for subfoveal hemorrhage: Prognostic factors and clinical outcomes
Read Dr Lapere’s published study A rare case of perfluoro-n-octane in the orbit following vitreoretinal surgery on the Canadian Journal of Ophthalmology website.